According to Autism Canada, “Autism Spectrum Disorder, or autism, is a neurodevelopmental disorder that impacts brain development causing most individuals to experience communication problems, difficulty with social interactions and a tendency to repeat specific patterns of behaviour. There is also a markedly restricted repertoire of activities and interests.”
Rising Incidence of Autism is Alarming
More children than ever before are being diagnosed with ASD. It is unclear how much of this increase is due to a broader definition of ASD and better efforts in diagnosis. However, a true increase in the number of people with an ASD cannot be ruled out. The increase in ASD diagnosis is likely due to a combination of these factors.
According to the U.S. Centres for Disease Control (Ref 1), the incidence of ASD was 1 in 59 children in 2014. This estimate is roughly 30% higher than the estimate for 2008 (1 in 88), roughly 60% higher than the estimate for 2006 (1 in 110), and roughly 120% higher than the estimates for 2002 and 2000 (1 in 150). There is no sign that this worsening trend is slowing.
ASD Characteristics
As its name implies, individuals with ASD may exhibit a spectrum of challenging behaviours.
Individuals with severe autism conditions may have serious cognitive disability, sensory problems and symptoms of extremely repetitive and unusual behaviour. This can include tantrums, self-injury, defensiveness and aggression. Without appropriate intervention, these symptoms may be very persistent and difficult to change. Living or working with a person with severe autism can be very challenging, requiring tremendous patience and understanding of the condition.
Individuals with mild autism conditions, however, may seem more like they have personality differences, making it challenging to form relationships.
The primary symptoms of autism include problems with communication and social interaction, as well as repetitive interests and activities.
Various Treatment Options
As one might imagine, with such a wide variety of factors like number and particular kinds of symptoms, severity (mild to severe), age, levels of functioning and challenges with social interactions, there is a wide variety of treatment options.
Approaches vary from intensive behaviour therapy, to education for both parents and children, to administration of pharmaceuticals (e.g., to suppress aggressive behaviour), to diet changes, to consumption of dietary supplements that address nutrient deficiencies. The options available to parents of an ASD child can be daunting. Autism Canada has some useful information about the evolving options. (Ref 2)
The basic problem is that, as with most modern chronic disease, treatments tend to address observed symptoms rather than trying to tackle underlying causes.
What Causes Autism?
Over the years there has been much research and speculation about the cause of ASD. There is even the possibility that, given the range of symptoms, there may be multiple different causes.
Some of this speculation has received sensational reporting in the news media. Who has not heard the claim by many parents that certain vaccines administered to young children provoked the development of ASD? This story has seen its ups and downs, involving emotional claims by parents and condescending reassurances from pharmaceutical companies. (I haven’t seen a really good response to the parents’ question of “why on earth would a pharmaceutical company include toxic mercury in a preserving agent for a vaccine directed at very young children, since its only function seems to be to save the company money by extending the shelf life of the vaccine?”) On the other hand, apparently valid studies have shown no correlation between vaccines and incidence of ASD.
But some relevant analysis seems to shed light, not just on the cause of ASD but also on a possible cause of a variety of other neurological disorders that have seen increasing occurrence trends in recent decades. Although this may be new to many people, this is not new research. The relevant science and analysis is well laid out in a report entitled “Environmental contamination and autism: Special report from UPHE”. UPHE is the Utah Physicians for a Healthy Environment and the report was published in January of 2015 (Ref. 3) I encourage you to read the entire report.
In addition, on Jan, 29, 2015, six physicians with expertise on how air pollution affects the brain gave a 75 minute presentation on the latest research on this critical public health topic. (Ref. 4) On that page is a link to the audio of the presentation and a summary of the highlights. For those with specific interest, I recommend it.
Quoting from the report:
In early 2014 leading scientists in pediatrics and public health warned of a “silent pandemic,” of brain disorders citing strong evidence that “children worldwide are being exposed to unrecognized toxic chemicals that are silently eroding intelligence, disrupting behaviors, truncating future achievements and damaging societies.”
These toxins — heavy metals, fluoride, chemicals like PCBs, toluene, solvents, flame retardants, BPA, phalates, pesticides, and PAHs (polycyclic aromatic hydrocarbons) — are found in the air you breathe, the food you eat, the water you drink, and the grass your kids play soccer on. Dramatically escalating rates of autism are part of this “silent pandemic.” Autism rates have climbed another 30% just since the last survey of two years ago, with Utah having the second highest rates of autism in the country, double the national average. As of 2012, one in every 32 Utah boys had autism. This “silent pandemic” warning should be a real wake up call for Utah physicians and policy makers.
Evidence is mounting that autism is likely caused by environmental exposures in genetically susceptible individuals. Supporting an environmental/genetic tag team are other studies showing autistic children and their mothers have a high rate of a genetic deficiency in the production of glutathione, an antioxidant and the body’s primary means of detoxifying heavy metals. High levels of toxic metals in children are strongly correlated with the severity of autism. Low levels of glutathione, coupled with high production of homocysteine, increase the chance of a mother having an autistic child to one in three. That autism is four to five times more common among boys than girls is likely related to a defect in the single male X chromosome contributing to antioxidant deficiency. But there is no such thing as a genetic disease epidemic because genes don’t change that quickly, so the alarming rise in autism must be the result of increased environmental exposures that exploit these genetic defects.
While numerous environmental exposures have been implicated, including pharmaceuticals like anti-depressants, in the last few years a growing body of epidemiological studies have been published linking autism to air pollution, including a highly regarded one from the Harvard School of Public Health just last month that showed a strong correlation between prenatal air pollution, especially in the third trimester, and autism.
Enhanced GSH Levels as a Key Countermeasure
If we look at the highlights:
- heavy metal and toxic chemical concentrations in the mother during pregnancy,
- heavy metal and toxic chemical concentrations in the ASD child,
- co-occurring conditions (Ref 5) that correlate to low glutathione levels, and
- oxidative stress as a common theme across the board
it becomes obvious that glutathione (GSH) is a critical factor.
If we review the various roles that glutathione plays in your body (refer to Why Does Your Health Depend on Glutathione) we can see a possible strategy. The major threat factors identified in the UPHE analysis are chemical toxins, heavy metals, oxidative stress and inflammation.
Glutathione:
- is the body’s master detoxifier, removing chemical toxins from the body,
- chelates a variety of heavy metals out of the body,
- is the body’s master antioxidant, neutralizing free radicals and thereby reducing oxidative stress, and
- reduces cellular inflammation.
The countermeasures seem obvious. Increase the body’s intracellular glutathione levels.
Possible Actions to Take
If we assume that the analysis published by UPHE is valid, there are a few things that you could do to protect against neurological harm, both for your baby and for yourself:
- If you are pregnant or considering pregnancy, take action immediately to increase your intracellular glutathione levels at least until you stop breastfeeding.
- If you are an adult, understand that this harmful pollution is also a risk to your health. Take action to increase your intracellular glutathione levels on an ongoing basis.
- If you have a new baby or young child, have their glutathione levels checked periodically. And if indicated, take action to increase their intracellular glutathione levels. Or consider doing this anyway as a general preventive measure.
- If you are an adult with ASD, your body is no doubt in a state of oxidative stress. Take action to increase your intracellular glutathione levels on an ongoing basis.
- Finally, get behind any initiative that will get governments to severely reduce industrial air pollution worldwide. It’s either that or get used to the idea of every individual, including young children, wearing a functional Darth Vader mask to help keep the toxic pollution out of their bodies.
References
Reference 1: https://www.cdc.gov/ncbddd/autism/data.html
Reference 2: https://autismcanada.org/living-with-autism/treatments/
Reference 3: http://uphe.org/air-pollution-health/the-brain/environmental-contamination-and-autism-special-report-from-uphe/ January 2015
Reference 4: http://uphe.org/air-pollution-health/the-brain/ January 2015
Reference 5: https://autismcanada.org/about-autism/comorbid-conditions/
#chronicdisease #autism #glutathione

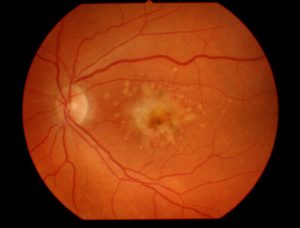 Recently I discovered that an online friend had been diagnosed with Age-related Macular Degeneration (AMD). My instant reaction was ‘I have something that I believe will help.’ But I decided to do a little research to be sure I had my facts right.
Recently I discovered that an online friend had been diagnosed with Age-related Macular Degeneration (AMD). My instant reaction was ‘I have something that I believe will help.’ But I decided to do a little research to be sure I had my facts right. This is a topic that is somewhat dear to my heart. My sister was diagnosed with Fibromyalgia a couple of decades ago. And her life has been miserable for much of that time.
This is a topic that is somewhat dear to my heart. My sister was diagnosed with Fibromyalgia a couple of decades ago. And her life has been miserable for much of that time. Post Traumatic Stress Disorder (PTSD) has probably been around for thousands of years. But it is only in the last hundred years or so that it has been recognized as a distinct psychological disorder. Its prevalence first came to public awareness during World War I. Front line soldiers in the trenches of Europe, who were the target of massive artillery barrages, were under constant stress, never knowing whether the next artillery round or bullet had their name on it. And this went on sporadically over several years.
Post Traumatic Stress Disorder (PTSD) has probably been around for thousands of years. But it is only in the last hundred years or so that it has been recognized as a distinct psychological disorder. Its prevalence first came to public awareness during World War I. Front line soldiers in the trenches of Europe, who were the target of massive artillery barrages, were under constant stress, never knowing whether the next artillery round or bullet had their name on it. And this went on sporadically over several years. Symptoms can include:
Symptoms can include: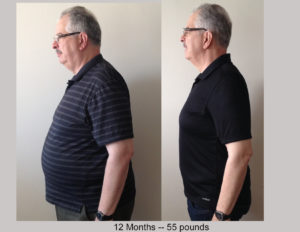 A few years ago my daughters started expressing concern for my health. They nagged and cajoled at every opportunity, telling me I needed to get in better shape. I knew they were right but I didn’t want to go to the effort to change. I would huff and puff going up a flight of stairs. I admit that I was a little overweight. (Alright, I’ll tell the truth. I was obese.) I paid a premium price for most of my clothes because I had to shop in a large men’s specialty clothing store.
A few years ago my daughters started expressing concern for my health. They nagged and cajoled at every opportunity, telling me I needed to get in better shape. I knew they were right but I didn’t want to go to the effort to change. I would huff and puff going up a flight of stairs. I admit that I was a little overweight. (Alright, I’ll tell the truth. I was obese.) I paid a premium price for most of my clothes because I had to shop in a large men’s specialty clothing store.