 On a couple of occasions I have asked my doctor about whether I should take a particular supplement. This seemed a good idea at the time since your doctor is supposed to be the ultimate expert when it comes to human health. What I expected was either “yes that’s a good idea because…” or “no, you shouldn’t do that because…” But the answers I got were neither.
On a couple of occasions I have asked my doctor about whether I should take a particular supplement. This seemed a good idea at the time since your doctor is supposed to be the ultimate expert when it comes to human health. What I expected was either “yes that’s a good idea because…” or “no, you shouldn’t do that because…” But the answers I got were neither.
Based on my research, the supplements I was asking about should have been beneficial. What I was seeking was confirmation, based on the doctor’s knowledge of my current health and the medications I was taking, that there were no counter-indications to me taking the supplement. What I got was waffling – no firm response either way. I found this quite disturbing. The responses left several impressions:
- I could take the supplements if I wished but the doctor would offer no opinion about what beneficial effect they might have.
- There was an underlying message that I might be wasting my money. He seemed to be saying that I should be able to get all of my needed nutrients from a healthy diet.
- The doctor seemed not very knowledgeable about the supplement despite the fact that the ingredients were clearly listed on the packaging.
In frustration I went to talk with my pharmacist. She gave me a very clear response. This and that ingredient in the supplement would likely lead to this benefit; there was no risk of harmful interaction with my current medications; but I should ensure that at least x hours separated taking this medication and that supplement to ensure no interference with the effectiveness of the medication.
So why wouldn’t the doctor, the supposed expert in my health care, give me a straight answer?
Physician Training
After research and some thought the answer has become clear. As a society we have this image of a doctor, promoted heavily by the medical profession, as the ultimate expert in human health. We assume anything a doctor says about human health is an absolute fact. But that is a false assumption.
A doctor goes through many years of education, training and practice that has a focus on two things: diagnosing injury and disease; and treating the injury or disease. Diagnosis consist of gathering information about the presenting condition (asking questions of the patient, taking physical readings such as temperature and blood pressure, running a number of tests, etc.), analyzing the information to develop a hypothesis about the condition, and formulating a treatment plan based on the hypothesis. Treatment typically involves administration of pharmaceutical drugs and possibly surgical intervention. That training and experience has very little to do with keeping you healthy. They should rightly not be called health care professionals but rather injury and disease treatment professionals.
When you ask a doctor a question that has a focus on maintaining and enhancing optimum health, the doctor has no basis for offering an informed answer because their training and experience has not addressed the topic in any meaningful way. Their entire mindset is on treating injury and disease. Their idea of preventive health care is diagnosing disease earlier rather than trying to prevent the disease in the first place.
Physician Risk Mitigation Strategies
When a doctor prescribes a pharmaceutical drug they must be very careful. And they know it. There is a very good reason for that concern. Almost all pharmaceutical drugs are toxic poisons. When given in small doses they may have a specific beneficial effect in certain circumstances. But prescribing the wrong drug or a patient taking too much of the drug can have serious and even fatal consequences. It is no wonder that one of the largest costs that a doctor incurs is malpractice insurance. They tend to be extremely cautious. And you can understand that position.
Also the pharmaceutical industry is highly regulated. Before a drug can be made generally available it must go through extensive clinical trials. The intent is to prove safe dosages and to verify effectiveness at treating a specific condition. The testing could take several years and cost hundreds of millions of dollars. The tests must be run again if the drug company wants to make any claims about it being useful to treat a different condition. The standard for these tests is placebo controlled blind testing involving a significant number of subjects. Given the risks represented by toxic pharmaceuticals, the rigor demanded is understandable.
Where the problem arises is the tendency of the medical community (pushed to some extent by the pharmaceutical industry) to think that the same risk and testing standards apply to nutritional supplements. That is a false assumption.
Unlike pharmaceutical drugs, nutritional supplements are not toxic poisons. That is why the regulatory authorities treat them differently.
To illustrate the point consider this. In the April 15, 1998 Journal of the American Medical Association, Dr. Bruce Pomeranz said, “The medications we prescribe cause over 100,000 deaths per year.” That’s prescriptions where the patient took the medication as instructed. He also stated that another 2.1 million patients have serious complications because of medications. The same paper pointed out that properly prescribed and administered medication is the fourth leading cause of death in the United States (Reference 1). In contrast, the number of deaths in any given year attributable to vitamin supplements when taken as directed is zero.
Despite this, doctors in general and many members of the wider population assume that because a supplement has the same physical form as a medication (a pill or a capsule) the same criteria should apply.
So it is not surprising that you won’t see many doctors endorsing any particular nutritional supplement. In fact in my jurisdiction, the College of Physicians and Surgeons (the licensing body for doctors) has stated that any physician that prescribes or recommends a compound that is not backed up by a peer reviewed placebo controlled blind study of the effect on a single specific condition risks losing their license to practice medicine.
To avoid risk of a malpractice law suit or loss of their license, doctors actively shy away from offering any meaningful advice when it comes to most nutritional supplements. And to avoid temptation, many doctors keep themselves intentionally ignorant of the subject matter.
Don’t Blame Your Doctor
Don’t blame your doctor for this state of affairs. Every doctor that I know truly cares about their patients and wants to help. But their training and ongoing education, funded in large part by the pharmaceutical industry, as well as the regulatory environment in which they operate, limits what they can do.
Sixty years ago doctors were treated like gods when it came to the human body. And the medical profession actively promoted that view. But now, with ready access to all manner of knowledge about health, disease, and many different approaches to enhancing our health, people are starting to take a more active role in managing their wellbeing. That is a good thing.
But please don’t go to your doctor with the the 1950’s view of their role and pester them about something that is outside their area of expertise. You will both come away from the experience very frustrated. The doctor will feel you have wasted his time that could be better spent treating a disease. And you will feel you have wasted your time and emotional energy because your concerns have been ignored. Accept the doctor’s role for what it really is (and not how the medical community would like it to be perceived).
What Can You Do?
It is a reasonable and prudent thing to do to seek professional advice before putting some new compound into your mouth. If you can’t get a straight answer from the medical professionals where can you go?
The obvious answer is to talk with your pharmacist. A pharmacist is an expert in understanding the effect that various chemical compounds have on the body and how different compounds might react or interfere with other compounds. They are far more knowledgeable than most doctors in this area.
When you approach the pharmacist, ensure that you have relevant information available:
- the ingredients list for the supplement in question,
- a list of the other supplements and medications you are taking, and
- any diagnosed conditions you may have.
The key question to ask is “do you see any problem with me taking this supplement?” Then based on the answer to that question and any other research you have already undertaken, make an informed decision. But don’t depend on your doctor to contribute in any meaningful way to this decision.
Reference 1: J. Lazarou, B.H. Pomeranz, P.N. Corey, “Incidence of adverse drug reactions in hospitalized patients,” JAMA, 279 (1998)
#health #science #nutraceuticals
 Yesterday I was in the gym change room just getting ready to go home after a workout. A fellow came in after finishing his workout. There was a light clunk when he opened his locker, a few down from mine. On the floor between us was a small bottle, with a protrusion at right angles out the side of the bottle. I asked if that was his puffer.
Yesterday I was in the gym change room just getting ready to go home after a workout. A fellow came in after finishing his workout. There was a light clunk when he opened his locker, a few down from mine. On the floor between us was a small bottle, with a protrusion at right angles out the side of the bottle. I asked if that was his puffer.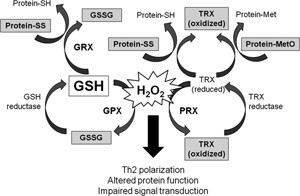 One of the conclusions seemed to be that if there is insufficient glutathione (GSH) available in the cell, the level of free radicals will increase. An imbalance represented by high levels of free radicals results in oxidative stress and cellular inflammation. This state of affairs diminishes normal cell function by interfering with internal cell signalling.
One of the conclusions seemed to be that if there is insufficient glutathione (GSH) available in the cell, the level of free radicals will increase. An imbalance represented by high levels of free radicals results in oxidative stress and cellular inflammation. This state of affairs diminishes normal cell function by interfering with internal cell signalling.
 Every living cell in your body has this miracle molecule. As with oxygen, water and fuel (food), if this molecule is absent from a cell the cell will die. If it is not at an optimum level the cell will struggle to do its work. This molecule is made by your body and every cell in your body needs it.
Every living cell in your body has this miracle molecule. As with oxygen, water and fuel (food), if this molecule is absent from a cell the cell will die. If it is not at an optimum level the cell will struggle to do its work. This molecule is made by your body and every cell in your body needs it. On a couple of occasions I have asked my doctor about whether I should take a particular supplement. This seemed a good idea at the time since your doctor is supposed to be the ultimate expert when it comes to human health. What I expected was either “yes that’s a good idea because…” or “no, you shouldn’t do that because…” But the answers I got were neither.
On a couple of occasions I have asked my doctor about whether I should take a particular supplement. This seemed a good idea at the time since your doctor is supposed to be the ultimate expert when it comes to human health. What I expected was either “yes that’s a good idea because…” or “no, you shouldn’t do that because…” But the answers I got were neither.